The Challenge
Osteoarthritis is a chronic disease suffered by many elderly patients. Though there is no cure for the disease, patients can slow its progress and improve their quality of life by changing their behaviour. Successful self-management of the disease also improves the chances that a surgical joint replacement, if required, will succeed. Biomet, a leading orthopedics manufacturer, asked designers at TU Delft to investigate ways the journey of these patients from primary care to surgical intervention could be improved.
The Outcome
A concept design for a data-gathering wearable which tracks osteoarthritis patients’ activities and symptoms, and helps them understand their illness and plan effectively to get the best quality of life. Inclusive graphics, using pictures and characterisation, were developed to help elderly patients to understand the data and make meaningful connections.
Skip to: User Research:Dealing with Osteoarthritis, Concept: Data-Gathering to Understand, Wearable Design, Inclusive Data Interface
Dealing with osteoarthritis: frustration & confusion
Osteoarthritis patients were interviewed not only about their illness but also about their lives, aspirations and activities. I wanted to know how the disease affected patients’ happiness and quality of life.
The happiest patients were those who had learned to recognise what physical activities caused them pain, and to maximise their quality of life by planning their activities carefully. For example, a patient who knew that long periods of standing caused her pain had learned to walk back and forth while working in the kitchen, and avoided standing up altogether on Saturdays so she could be sure of going to her church group on Sundays. Thus, though she could not cure the disease, she could ensure the best quality of life in spite of it.
Other patients, however, would find it difficult to correlate their activities with their symptoms, since there is often a time delay before symptoms begin. Rather than planning with their illness in mind, they would fight against it, becoming frustrated and unhappy when it prevented them from doing things they had planned.
These difficulties made it hard for patients to follow the “self-management” advice given by GPs (along with prescribed painkillers) after diagnosis. Patients did not regard this prescription as ‘real’ treatment, and thus were reluctant to return to the doctor until their pain became unbearable, at which point the optimal stage for joint replacement had passed.
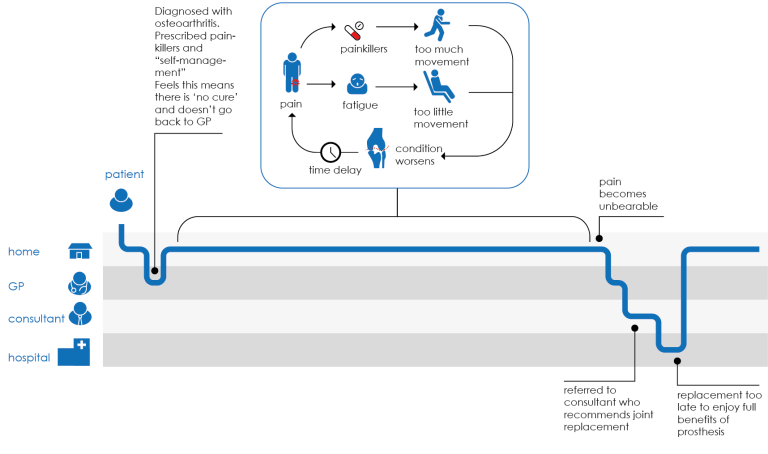
Our design goal became to help patients understand their illness and to increase trust in self-management prescriptions, resulting in a better patient journey where the patient makes regular contact with the health system and joint replacement surgery is performed at the optimal time.
Data-gathering to understand
A concept was developed for a wearable device which could track patients’ physical activity and their pain symptoms, helping them figure out how to plan their activities in order to minimize symptoms.
This wearable would be prescribed by the GP after diagnosis as a ‘self-management’ aid, providing a tangible treatment and improving patient trust. The patient would then use it to track their activities and level of pain, and the GP and patient would review this data together to figure out the best self-management plan for the patient. The wearable device could also be continually worn to track symptoms in the long term and help the GP discern when surgical intervention is needed.
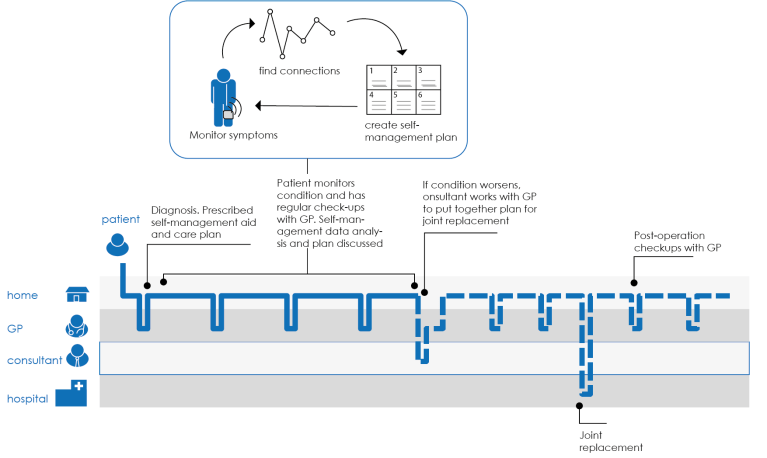
User research was performed to find the best way to both collect and display the data which characterised a patient’s condition. A two-pronged approach was taken; patients were shown iterative designs, in storyboard form, of different ways data could be gathered. At the same time, contemporary technology for activity monitoring was investigated to see what was most suitable for the kind of data required.

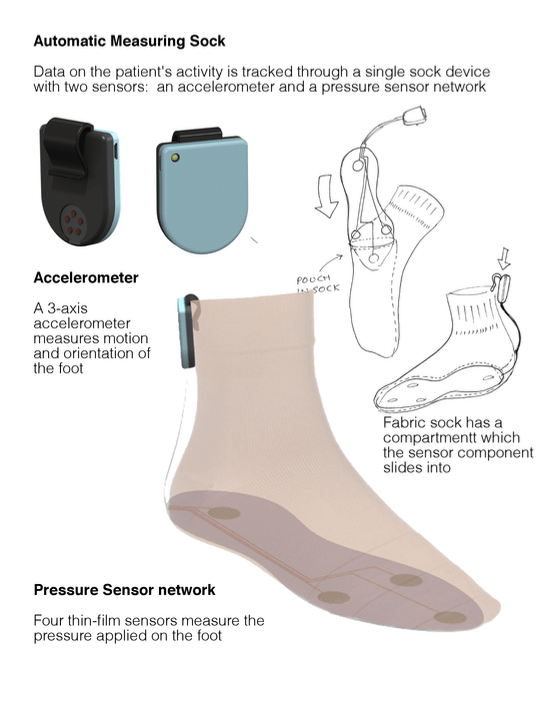
Many existing commercial wearables are inappropriate for measuring activity relevant to osteoarthritis since they are not able to measure increases in the amount of weight the wearer is putting on their feet (for instance, by carrying bags or climbing stairs). Since weight is a key aggravating factor for osteoarthritis, a design was chosen consisting of pressure sensors in the sole of the foot and an accelerometer on the ankle, which together could measure force through the leg and analyse gait and range of movement.
Wearable Design
Since pain can only be measured subjectively, an ”activity sampling” method was chosen, similar to that often used in research studies. The user is alerted at random intervals in the day and asked to give a simple indication of their pain level – in this case a wristwatch with pain levels from 1-5. The simple dial configuration was chosen to make the design accessible to patients with limited dexterity.
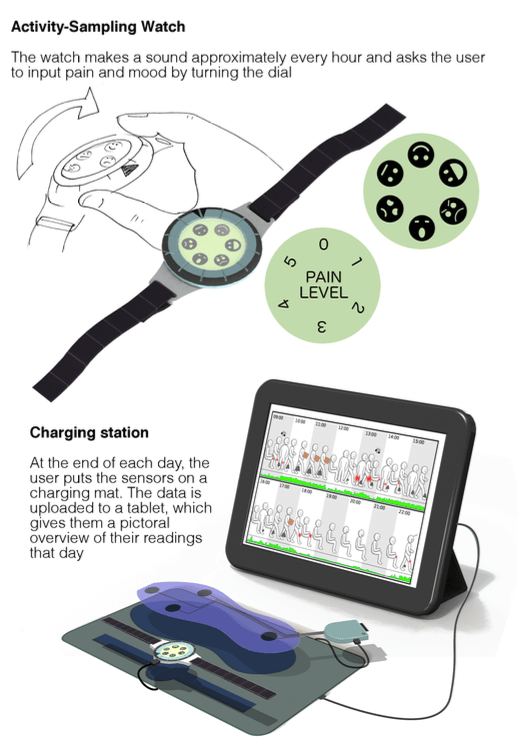
Making sense of the data
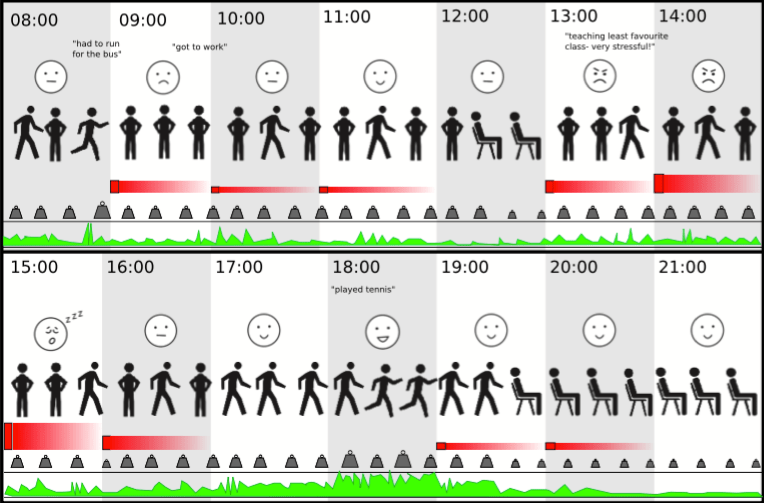
Though patients liked the idea of having access to the data, they found conventional means of displaying it – graphs and numbers – confusing and unhelpful.
To make comprehension easier, picture-based graphics were created to make the data seem less like a stream of numbers and more like a narrative story. Different types of data representation were developed – from basic pictographs to illustrations in the style of a comic strip (see below) – and tested with users alongside traditional data presentation. Users were asked to interpret the symptoms shown and find correlations between activity and pain. The stronger the visual narrative, the better patients were able to describe trends in the data.